Tag Archives: therapy
Last year, I wrote a post a day for Prematurity Awareness Month. On Prematurity Awareness Day, I wrote a post titled “Why Have Prematurity Awareness Day (or Month)? This year, I’ve stared at a blank screen for nights. I tell myself that I’m waiting for a muse of fire.
If the truth be known, I’m sick and tired of prematurity. Two and a half years after Charlie’s early arrival, not a day goes by that it does not impact my life in some way. Additionally, I think about it several times a day.
No, I’m not obsessive. It’s just that my life revolves around prematurity.
For starters, I am constantly problem solving with doctors, therapists, nurses, and pharmacies. Then, there is the hassle of social services. Charlie’s medicaid waiver should have been decided months ago. Plus, the insurance company likes to waste my time with automatic denials or by providing misleading information. That’s just the obvious stuff.
Prematurity creeps into my “regular” parenting life. If I hear a cough, I cringe and make a quick escape with Charlie. No need to challenge those preemie lungs. Feeding… oh goodness… let’s not get into feeding. During play, I watch to see if her pincer grasp is improving, if a heel strike will miraculously appear while she’s walking, and if she favors her left side as usual.
Currently, I’m stressed about Charlie’s upcoming MRI because it has to be performed under sedation with all the risks it entails. Additionally, I’m trying to schedule her new AFOs (yes, she’s being prescribed orthotics AGAIN) before the end of the year since our deductible has been met. On top of it all, meal time is a juggling act of mentally calculating her caloric intake while coaxing her to eat.
Truly, I think about prematurity many times a day. My brain refuses to contemplate it further and my thoughts about it have been tapped out.
But, that’s why I need to write about it. If, for anything, so that our story is told.
So that people don’t make the mistake of thinking that preemies are just small babies. So that people don’t believe that babies come home from the NICU and are suddenly “fine”. So that people know that some preemies don’t ever catch up and some never come home.
We can do better.
For example, we can fund more research, lobby for better health care policies, and educate more people. By doing so, we can improve the lives of these babies and of parents like me.
I’m very hopeful about Charlie’s future, but I’m tired of prematurity. Everyone else should be tired of it too. Let’s do something about it.

5 Comments | tags: baby, hope, Life, march of dimes, medicine, micro preemie, nicu, parenting, preemie, therapy | posted in Blog, Celebrate, Premature Birth, Special Needs Parenting
I had a feeling it was going to be a great semester for Charlie’s speech. I knew in the second week that Charlie’s student therapist understood Charlie. As sweet and cute as Charlie is, she is highly energetic and difficult to focus (more so than most two year olds). She can be a handful.
By the second week, the student therapist had learned to work with Charlie amazingly well. I was impressed.

This is what part of the screen looks like when I watch from the observation room.
For most sessions, I sit in the observation room with the other parents and watch the session over the cameras on a computer screen. I did this initially in case Charlie became unruly or melted down. I wanted to be able to rescue the student therapist if needed. Now, I just sit there, read, and occasionally glance up at the screen.
What goes on during speech therapy? A variety of play activities. Each semester, I’m always impressed by the students.
If Charlie starts to run circles in the room, the student therapist patiently says, “Oh, you need to run? OK, lets go to the sensory room and bounce on the trampoline.” While Charlie bounces, the student therapist sings a song about bouncing with her.
In another activity, Charlie pretends to shop and has to ask for each item she wants to put in the cart. In Charlie’s favorite activity, she plays basketball where she has to ask for the ball and to be lifted up to the hoop with “Want up!”.
Last session, she played a considerable amount of time with a fake ice cream cone. I noticed it when I looked up at the screen. I thought it was odd because Charlie has never really had ice cream. She gets the non dairy stuff when we go get ice cream. Not the type of ice cream she was playing with while learning to say “ice cream”.
Later that evening, Charlie, Charlie’s dad, and I grabbed a quick bite to eat. After we were finished, we passed the yogurt store where Charlie gets her non dairy treat. She pointed and exclaimed, “W-want ice cream! Ice cream!”
I was stunned.
We actually understood what she was saying! How did she make the connection that her non dairy treat in a cup was the same as that creamy looking cone she played with earlier?
We were obligated to follow our rule. If Charlie uses her words to ask for something, she gets it. She got her non dairy version of ice cream that evening.
Overall, I’ve noticed significant improvement with her speech. Charlie experiments more with two word phrases such as “Bye daddy!” and we can understand more of what she says.
Feeding is finally moving forward as well. With the introduction of erythromycin, she eats more than two bites, doesn’t vomit, and her reflux is gone. She still has difficulty tolerating some textures and with chewing food. However, I’m relieved that she is no longer stuck.

5 Comments | tags: developmental delay, family, feeding, hope, Life, love, micro preemie, micropreemie, parenting, preemie, premature birth, special needs, speech therapy, therapy, toddler | posted in Activity, Developmental Delays, Special Needs Parenting, Speech Therapy
Charlie and I made the two hour pilgrimage to the university health system that houses her specialty clinics. Today’s topic of concern was feeding. I tend to be leery of new specialists since our meeting with the physiatrist from another health system. In most cases, like today, being wary is unwarranted.
Today’s feeding consultation was with a gastroenterologist and speech therapist whose expertise is in feeding. For those who don’t know, Charlie has overcome a significant oral aversion. However, she feeds poorly and continues to be (partially hydrolyzed whey protein) formula dependent.
 At the beginning of the appointment, we discussed Charlie’s feeding history and GI issues. Charlie was physically examined and her previous test results (swallow study and other imaging) discussed. Later, they watched Charlie eat (as much as she would) foods of different textures and consistencies. At the end, we discussed what may be the issues and a plan.
At the beginning of the appointment, we discussed Charlie’s feeding history and GI issues. Charlie was physically examined and her previous test results (swallow study and other imaging) discussed. Later, they watched Charlie eat (as much as she would) foods of different textures and consistencies. At the end, we discussed what may be the issues and a plan.
From the GI perspective, Charlie has slow motility due to her CP. Her stomach empties slowly and things continue to move slower than usual through her intestines. She also has a milk protein allergy which is common among preemies.
From the speech/feeding perspective, Charlie does a poor job of chewing. Despite the appearance of a chewing motion, she mostly uses her tongue and sucks food to mush rather than chew it. In addition, she has sensory related issues such as stuffing, a preference for strong flavors, and a gag reflex that is more sensitive than average.
All of these things, hamper her feeding progress.
The gastroenterologist has suggested Charlie stop using infant formula. It is no longer appropriate. Instead, she will start a “big kid” partially hydrolyzed whey protein formula with fiber. It is 30 cal/oz as opposed to the infant 20 cal/oz. The fiber will help with her motility issue. Possibly, the lower fluid intake will make her feel less full and stimulate appetite.
The speech/feeding suggestion is to go back to using soft foods, easily chewed foods, or finely cut up foods (almost pureed). The hope is she will not have to work as hard at chewing and will ingest more than just a couple of bites. Over time, with work and practice, her jaw muscle strength and coordination will improve. The feeding specialist will send some suggested foods and exercises.
Overall, I was very pleased with how today’s consultation went. I felt like the professionals understood where we were with Charlie’s feeding and are supportive. I didn’t feel pressured to try things (like stopping the use of formula) that Charlie isn’t ready for. Plus, I feel like the treatment plan is realistic and doable. The frustration I’ve felt most recently over feeding has been abated.
Today’s appointment was a step forward after being stuck for some time now. I feel optimistic that Charlie will be a good eater sooner rather than later.
1 Comment | tags: baby, family, feeding, Life, medicine, micro preemie, mom, parenting, preemie, special needs, speech, therapy, toddler | posted in CP, Developmental Delays, Premature Birth, Special Needs Parenting, Speech Therapy, Uncategorized
For over a year, Charlie has attended at least one therapy appointment every week. Now, she has therapy four out five days during the work week. Mix in the appointments with the specialists and it becomes A LOT.
I’ve heard of and talked to parents whose kids have taken breaks from therapy. From time to time, I’ve secretly fantasized about it. But, I was afraid to. I didn’t want to miss out on opportunities. After some thought, I decided Charlie and I would take this week off of therapy.
It has been wonderful.
Rest assured, we aren’t sitting around the house and watching TV. We are getting out and doing things on our accord. We have no schedule to keep or places we have to be. We aren’t thinking about the goals she needs to work on. The freedom and relaxation has been fabulous. It’s like we’ve been on a vacation of sorts.
We are only midway through the week and are having a fabulous time.


Pictures from part of today’s adventure. It was Charlie’s first time on the playground merry go round.
5 Comments | tags: break, hope, Life, love, parenting, play, preemie, special needs, therapy | posted in Activity, Developmental Delays, Special Needs Parenting
Wow, March is busy! March is also National Cerebral Palsy Awareness Month. Just as with all the other month long celebrations, I am sharing Charlie’s story.
I knew there was something “not quite right” about the way Charlie moved when she had been home from the NICU for a few months. Her hands didn’t open when they should have, she missed all of her motor milestones at her adjusted age, and she was incredibly rigid when she slept. I begged the pediatrician for answers and she started Early Intervention.
Charlie was supposed to be one of those super preemies that left the NICU and never looked back. Because her NICU head scans appeared fine, we were not warned that cerebral palsy was a possibility. It was never discussed with us.
 I was blindsided by the delays and did my own research. My best guess concluded we were most likely dealing with cerebral palsy. I learned from my research we could help her. I just needed someone to tell me how.
I was blindsided by the delays and did my own research. My best guess concluded we were most likely dealing with cerebral palsy. I learned from my research we could help her. I just needed someone to tell me how.
Shortly after she missed her milestones, Charlie saw a developmental pediatrician. Although he did not diagnose her initially, he prescribed PT, OT, and feeding therapy. Charlie received her diagnosis of spastic diplegia at about eighteen months. Prior to that, I connected with another mom of a girl with cerebral palsy that has been an incredible support and resource (Thanks, Nicky).
After a couple months of therapy, Charlie’s hands opened and she could hold a toy. She learned to roll over a few months later. Things continued to progress with plenty of hard work and lots of therapy. She is now mastering walking. However, the multitude of therapies continue.
Cerebral palsy is a disorder that is a spectrum and affects each person differently. If there is one thing I want other parents of children newly diagnosed with CP to know, it is don’t give up hope. A diagnosis is helpful in order to receive services and understand the nature of the delays. It does not necessarily predict the future.
I’ve been amazed at how far Charlie has come and how much she can do.

2 Comments | tags: cerebral palsy, developmental delay, family, hope, Life, micro preemie, parenting, preemie, special needs, therapy | posted in CP, Giving Back
Despite my fear and anxiety, my surgery went well yesterday. Actually, the pain over the past few months was worse than the surgery. Currently, I am resting so I don’t reopen my wounds or restart any bleeding.
Today’s post is a guest post (written before my surgery) that can be found on JAM Sessions: Lessons Learned Through A Micro-Preemie. The post Seven Sensory Sensations is part of the blog’s brilliant Surviving Isolation series.
Enjoy!
Leave a comment | tags: activities, developmental delay, family, micro preemie, preemie, premature baby, premie, special needs, therapy | posted in Guest Posts
Today was one of those days. The weather was of the worst kind. The roads were icy enough to prevent us from going anywhere and there wasn’t enough snow to play in. What is a parent to do with an active toddler on days such as today? Unfortunately, this isn’t the first time it has happened. This time, I was ready. Here are a few of the activities I was armed with:
1) Kid’s meal toy bin: Charlie has yet to realize that most kids meal come with a cheap toy. Instead of giving it to her immediately, I keep the toys in a bin in the closet. On days like today, Charlie loves to dig through the bin and explore the “new” toys.
2) Finger painting with food: This is a sensory play idea from her therapist. While seated in her high chair (to contain the mess as much as possible), Charlie is presented with yogurt, ketchup, apple sauce, and whatever food “paint” that is handy. She enjoys spreading the condiments around the tray and will sometimes taste them.
3) Playing with dough: These recipes are kid safe and simple to make. I usually have the items around to make one of the three recipes.
4) Play with boxes and packaging: We use online ordering often enough that we usually have a box or two waiting to be recycled. If the box is big enough, I show Charlie that she can climb in and out of it or make a tunnel to crawl through. For the smaller boxes, Charlie likes to put small toys in and take them out. The bubble wrap and other packaging that is frequently included with the boxes are added fun accessories.
5) Musical Accompaniment: Charlie has a toddler musical instrument set. But, her favorite is the simplest and cheapest to make. When beans, rice, cereal, or whatever is on hand is added to a closed container it makes a drum and a shaker. I construct a play list of different types of music. Charlie likes to shake the instrument, sing, or dance to the different kinds of music.
6) Explore Different Textures: I fill a clothes basket with different textured fabrics and items. At first, I let Charlie explore it on her own. Later, I sort through it with her. We discover different textures as I ask, “How does it feel? Is it rough? Is it soft? Is it scratchy?” Often, we end up playing peek a boo with the different fabrics.
7) The Straw Game: This is another idea that came from Charlie’s therapist. In order to work on Charlie’s oral motor skills, I present thicker substances to her with a straw. She likes to suck up apple sauce, jello, yogurt, pudding, and other thicker liquids.
8) New Story: I find a book that Charlie hasn’t read yet or hasn’t read in a while (library books are great for this). I present it to Charlie and let her look through it first (if she is interested). Afterwards, we read it together.
9) Bowling: I use plastic soda bottles out of the recycling bin and put a little rice or beans in the bottom. Charlie likes to knock them over. However, I’m trying to teach her to use a ball to do so.
10) Indoor Bubbles: Depending on the indoor interior, this may or may not be a good idea. I blow bubbles with Charlie. She works on blowing (I still blow the majority of the bubbles), she pops the bubbles in the air, or steps on them if they reach the floor.

Charlie finger painted today with hummus, yogurt, and strawberry apple sauce.
5 Comments | tags: activities, developmental delay, Life, micropreemie, parenting, play, preemie, premie, special needs, therapy, toddler | posted in Activity, Developmental Delays, How To..., Occupational Therapy, Physical Therapy
Lately, many readers have expressed curiousity about Charlie’s music therapy. In the following post, I try to answer the questions that have been asked.
After lock down last year, Charlie and I ventured to her first baby group. It was an experiment. She had serious sensory issues and her motor skill progress was at a stand still. I was looking for more ways to stimulate her in addition to Early Intervention. To my surprise, the baby group session went well… especially the musical portion.
 Inspired by the success, I scoured the internet for a local baby music class. My web search led to a local non profit organization called The Community Music School of The Piedmont. The music school offers music therapy and a Music Together class as well as other programs.
Inspired by the success, I scoured the internet for a local baby music class. My web search led to a local non profit organization called The Community Music School of The Piedmont. The music school offers music therapy and a Music Together class as well as other programs.
Charlie was almost a year old but had the motor skills of a four month old. I was not sure she could keep up with the rest of the Music Together class. Plus, I was concerned about her low sensory threshold. I sent an email to the school and asked which program would be the best fit for Charlie. The response was an invitation to sit in a Music Together class and to meet the music therapist. After Charlie and I met the music therapist, I immediately knew that music therapy was where she belonged.
Every Wednesday for the last nine months, Charlie has attended music therapy. She has benefited in several ways.
First, her sensory threshold has improved. The therapist has actively worked with Charlie on improving her tactile defensiveness and auditory tolerance. Charlie likes to feel the vibrations as she plays the drum, while the therapist plays the guitar, or the time a cello was played in her presence. The therapist also uses feathers, scarves, stuffed animals, and a bead bag in the musical play. 
Additionally, her motor skills have progressed. There have been a few times when something was not registering with Charlie in PT or OT. For whatever reason, she did not understand the skill the EI therapist was trying to teach. The music therapist teaches similar skills using musical instruments. In music therapy, it is like seeing a light bulb go off above Charlie’s head as she understands and performs the skill for the first time.
Finally, Charlie’s speech development has benefited from the music therapy. Before Charlie 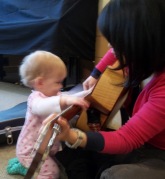 learned to open her mouth to vocalize sounds, she grunted to fill in a pause while the therapist sang. Now, she tries to fill in a missing word with the few sounds she has mastered. Charlie started “singing” before she tried to talk.
learned to open her mouth to vocalize sounds, she grunted to fill in a pause while the therapist sang. Now, she tries to fill in a missing word with the few sounds she has mastered. Charlie started “singing” before she tried to talk.
Whether Charlie progresses to learning an instrument or not will be a choice left up to Charlie. Music therapy is right for us. Charlie enjoys music therapy and gets quite a bit out of it. Sometimes, she says, “Yay!” when I pull the car into the school’s parking lot.




1 Comment | tags: developmental delay, early intervention, family, Life, micropreemie, music, music therapy, parenting, preemie, special needs, therapy | posted in Activity, Music Therapy, Occupational Therapy, Physical Therapy, Speech Therapy
As if things weren’t stressful enough, Thursday evening our furnace gave out. We are cramped into a hotel room while the furnace is replaced. The situation is not ideal but it is not bad. We have been making the best of things and that includes enjoying the indoor pool.
 A year has passed since we have stayed in a hotel with Charlie. She is scared of the elevator and is obsessed with the trashcan. Overall, she’s been well behaved. I can contribute much of that to the indoor pool and Charlie’s swim class.
A year has passed since we have stayed in a hotel with Charlie. She is scared of the elevator and is obsessed with the trashcan. Overall, she’s been well behaved. I can contribute much of that to the indoor pool and Charlie’s swim class.
I have written about Charlie’s mommy and me swim class she started earlier this month. Charlie loves the class. I, on the other hand, have to confront my public pool aversion and bungle out of a swim suit as I prevent Charlie from crawling through the puddles on the locker room floor. Just typing that makes me wince.
This weekend, I realized the many benefits of Charlie’s swim class. I knew that it has helped her progress towards walking, it is helping her get stronger, and has developed better body awareness. But, I did not know that I was learning from the swim class.
We have had Charlie in the pool each day of our stay to burn off excess energy.
Charlie’s dad took her for the first swim. He had no idea what to do with her once he was in the pool. I suggested many of the  activities and songs from swim class. Charlie gleamed as they played. She showed how she could splash, kick, and “swim”. I showed her dad how to hold her in the pool. I know it sounds ridiculous. But, without the class, I don’t think we would have known how to get anything out of pool time with Charlie.
activities and songs from swim class. Charlie gleamed as they played. She showed how she could splash, kick, and “swim”. I showed her dad how to hold her in the pool. I know it sounds ridiculous. But, without the class, I don’t think we would have known how to get anything out of pool time with Charlie.
So yes, I hate having to lug everything to the pool for class. I am grossed out by public pools and the puddles in the locker room. I am exhausted by the time I haul Charlie up the stairs after class like a sack of potatoes. However, I’m glad that we are taking the mommy and me swim class and am pleased with the results. While it has been obviously beneficial for Charlie, it has its surprising pluses for me.
If anything, Charlie is one more step towards walking.
1 Comment | tags: developmental delay, family, hope, Life, love, micropreemie, parenting, preemie, special needs, therapy | posted in Activity, Physical Therapy, Special Needs Parenting
The developmental pediatrician has stated that Charlie is the type of baby the Early Intervention system was made for. I have no doubt that her participation in Early Intervention is a key reason as to why she is doing so well. While it works well for Charlie, I question if I am the type of parent Early Intervention had in mind.
Charlie has participated in the program for over a year and I am burned out.
I have not been feeling well since Thanksgiving. Caring for a child when feeling run down and ill is tough. It is about all I can handle. I don’t want the additional burden of having to actively participate in her multitude of therapy sessions. Nor, do I want to be responsible for her on going therapy.
While I really like a couple of her therapists, I don’t want regular visitors. Even my friends don’t visit frequently or a regularly. These regular early intervention visits feel intrusive. It feels like we are under the microscope even though I know we are not. It is like we’ve traded off part of our privacy for therapy services.
If I feel this way because I’m under the weather, it makes me wonder how working parents feel about EI. Are reasons like these why other parents take “vacations” from therapy?
I know it is important that Charlie receive her therapy services. I am not sure if the current is still the way that is right for us.
Questions for special need parents: Have you taken a break from therapy? Did you change things up? What works for you?

10 Comments | tags: early intervention, family, micropreemie, parenting, preemie, special needs, therapy | posted in Developmental Delays, Occupational Therapy, Pediatrics, Physical Therapy, Special Needs Parenting
For our newest adventure close to home, Charlie will be attending swim class which starts this week. We were able to find a really good deal on a mommy and me swim class. Pluses to taking the class include: Charlie loves the water and it will help her progress on her therapy goals.
There is only one problem… I am not a fan of public water facilities. It grosses me out. I don’t even like baths because I don’t want to sit in the dirt, oil, and germs I’m washing off of my body.
Since we have the opportunity to do something Charlie loves at an affordable price, I tried to tell myself I’m being silly. I thought that I was letting the germaphobe preemie mom instinct get the better of me. To reassure myself, I consulted with the University of Google. The CDC fact sheet I found was not very comforting.
Basically, I’m going to have to step way outside my comfort zone for this. That is the thing about raising Charlie. She challenges me to be braver, better, and try things I’m not comfortable with.

2 Comments | tags: family, micropreemie, parenting, preemie, recreation, swimming, therapy | posted in Activity, Physical Therapy
The holidays are speeding towards us and we are on a tight budget. Like many families with kids that have special needs, we have added financial demands such as orthotics, endless co-pays, therapies, and special formulas. I want Charlie to have a great Christmas but need to budget when the opportunity presents itself.
By scouring the web, I’ve discovered that I can save money on stocking stuffers while giving Charlie things she will enjoy playing with. These are the ideas that I’m using for Charlie’s stocking stuffers.
NOTE: Please keep in mind that item size is an important consideration in order to prevent choking hazards. Always supervise children appropriately.
1) Pipe Cleaners These are great because they serve many purposes. The odd texture can be used in sensory play. To work on fine motor skills, she can bend the pipe cleaners to create shapes or put them in a container.
2) Giant Buttons Due to Charlie’s petite size, her hands are often too small for “typical” toys. She enjoys playing with things that fit her tiny hands. She can place the buttons in containers, dump them out, sort them, or whatever ideas she comes up with.
 3) Cups I plan on browsing the shelves of the local dollar store for cheap plastic cups. Charlie likes to bang cups together, fill and dump them, nest them, stack them, and use them in water play. It is an added bonus if I can find cups with removable lids. Cut holes in the lids create more of a challenge for Charlie when she puts things in the cups.
3) Cups I plan on browsing the shelves of the local dollar store for cheap plastic cups. Charlie likes to bang cups together, fill and dump them, nest them, stack them, and use them in water play. It is an added bonus if I can find cups with removable lids. Cut holes in the lids create more of a challenge for Charlie when she puts things in the cups.
4) Craft Pom Poms This is another idea that is great for sensory play. Again, the possibilities for play are endless.
 5) Squeaky Animals and Ninja Ducks Charlie loves her small rubber squeaky toys and ninja ducks. She will be receiving more of these.
5) Squeaky Animals and Ninja Ducks Charlie loves her small rubber squeaky toys and ninja ducks. She will be receiving more of these.
6) Bag of Feathers These provide more sensory play and exploration opportunities.
7) Magnetic Alphabet Letters Charlie plays with the refrigerator magnets almost obsessively. This is an extension of that idea. In addition, Charlie’s dad has a magnetic write on/wipe off board in his office that will compliment this gift nicely.
 8) Shakers Charlie loves the maracas at music therapy. This idea was drawn from that.
8) Shakers Charlie loves the maracas at music therapy. This idea was drawn from that.
9) Pieces of Textured Fabric I’ve raided the scraps bin at the local fabric store. I’ve cut the scraps into equal size squares. I’m sewing together the corduroy, felt, taffeta, calico, velvet, fleece, etc to make a “book” of fabrics. Despite her tactile defensiveness, she is curious about different textures. I haven’t decided whether or not I’m going to spay the pieces to add scent.
10) Giant Beads Like most things on this list, these have many uses. She can work on fine motor skills by threading pipe cleaner through the beads. She can sort, learn to count (eventually), or make a shaker with the beads.

Leave a comment | tags: baby, christmas, crafts, developmental delay, family, gift, micropreemie, play, preemie, sensory, special needs, therapy, toddlers | posted in Activity
Today, friends from Colorado were in-state for a visit. The weather was rather warm for our meet up at a state park (that makes sixteen!). After a short play date, Charlie, Kaia, my husband, and I took a walk. It was followed by a splash in the lake. Her enthusiasm for digging in mud and splashing (she placed herself in the lake) is vast improvement from the first time she played in the river earlier this past spring. Overall, there has been remarkable progress with her sensory issues.


At home this evening, Charlie was all smiles for feeding therapy. We did not get a lot of therapy done but we laughed quite a bit (which is just as important).




Leave a comment | tags: baby, development, family, nicu, parenting, preemie, therapy | posted in Activity, Outdoors
From the moment I was hospitalized with pre-eclampsia at twenty four weeks, I found that I had much to learn rather quickly. It started when I had to learn what pre-eclampsia was and continued through out preemie life. Even now, I am still learning. Here are ten things that I learned about life from having a preemie born at twenty six weeks.
1) Frequently, things just happen. I used to think that less than ideal outcomes had a cause. After my time spent on the High Risk Perinatal floor and in the NICU, I realize that many times there is no rhyme or reason to how things play out. Now, I understand the meaning of “C’est la vie!”
2) Heroes don’t always wear capes. Sometimes they wear scrubs (as is the case of NICU nurses) and other times they are disguised in street clothes (like Charlie’s therapists or other people who show unexpected kindness).
3) Perfect does not always mean flawless… especially when used in the context of people. Quality of life is independent of ability.
4) Fight and fight like hell. Do not give up. Whether I’m advocating for Charlie or struggling with limitations forced upon us, most battles can be won in some way. If I lose, at least, I tried.
5) Be selective in choosing disputes and people. Caring for Charlie, managing her appointment schedule, running the household, and recreation time exhausts me. Many days, I feel like I’m barely keeping up. I have to be selective in where and with whom I invest my time and energy. I prefer to be with people and do things that rejuvenate me rather than those that further drain me.
6) My definition of “important” has changed significantly. Most of what was important to me before having a preemie is now trivial. 
7) Other than matters of life and death, most things can be managed or fixed. Some things just take more time than others.
8) Remember to breathe. There is nothing wrong or shameful in saying, “I need alone time.”
9) Laugh often… particularly at myself.
10) People can (and will) surprise and amaze me… that includes myself.
4 Comments | tags: baby, developmental delay, infant, medicine, mom, nicu, nursing, parenting, preemie, special needs, therapy | posted in Guest Posts, NICU, Premature Birth, Special Needs Parenting
Every week Charlie works on PT, OT, speech/feeding therapy, and attends music therapy. She frequently has specialist appointments or sees her regular pediatrician on the days without therapy. In the quest to solve Charlie’s mystery feeding issues, additional appointments and specialists are scheduled. I hit a wall last night. What is a mother to do when that happens?
Desperate for a break, I trimmed the scheduled appointments to a bare minimum the rest of the week (two left after today). This afternoon, Charlie and I went to the park to meet up with my moms group.
It was exactly what Charlie and I needed.
Charlie was delighted to have another opportunity to play with more kids. I was rejuvenated by the conversation from the other moms. Not only do I get ideas, understanding, and solutions from the other moms but I’m able to feel normal and have a sense of belonging. Inclusion is something that I have struggled with since Charlie’s birth. I finally feel like we belong somewhere. That is a really big deal. Especially, on days that I need downtime such as today.
After our trip to the park today, I feel less weary. Charlie has two appointments left this week to address her feeding difficulties. I’m hopeful we will receive some useful information. For morale’s sake, I need a tiny bit of progress or promise so I can resume the rigors of our regular schedule.
What do you other moms do when you burn out?

Charlie playing in the park today.
1 Comment | tags: baby, developmental delay, family, Life, medicine, micropreemie, mom group, nicu, parenting, preemie, special needs, therapy | posted in Developmental Delays, Occupational Therapy, Physical Therapy, Speech Therapy
This will be a quick post. I am in the midst of running errands (sitting in a waiting room) in preparation for the busy week ahead. Our week ahead will start off somewhat stressful and will end in relaxation.
First, there is Charlie’s NICU reunion. Earlier this month, I have written about whether or not we will attend. I have decided to attend and tomorrow is the big day. I must admit that I am a little nervous and uneasy about the reunion. Because of this, I have recruited a friend to go with Charlie and me.
Next, Charlie has an appointment for a follow up evaluation with the developmental pediatrician clinic on Monday.
In April, Charlie was assessed to have the skill set of a four to five month old. With her recent progress, I hope she is assessed at the ten month level in gross and fine motor skills. If so, she will have reached the minimum expectations for her adjusted age.
Despite her motor skill success, she is still significantly delayed with speech and feeding. I am optimistic they will have some useful suggestions. While I am hopeful about the appointment, I am a little fearful of being blindsided by an unexpected issue.
From the middle of the week on, we will visit a few state parks. It will be nice to have some relaxation and bonding time. I like the fact that it is a week off of therapy appointments.
Overall, I am trying to think about the holiday as little as possible this year. It was around the 4th last year that Charlie had her NEC scare. This year, I want to make happy memories that I will think about in the future when I think of the fourth.
I have my fingers crossed that we have an enjoyable and uneventful week ahead of us.

This sweet picture was taken by Monica DeMariano.
Leave a comment | tags: baby, developmental delay, family, nicu, preemie, special needs, therapy | posted in Developmental Delays



 At the beginning of the appointment, we discussed Charlie’s feeding history and GI issues. Charlie was physically examined and her previous test results (swallow study and other imaging) discussed. Later, they watched Charlie eat (as much as she would) foods of different textures and consistencies. At the end, we discussed what may be the issues and a plan.
At the beginning of the appointment, we discussed Charlie’s feeding history and GI issues. Charlie was physically examined and her previous test results (swallow study and other imaging) discussed. Later, they watched Charlie eat (as much as she would) foods of different textures and consistencies. At the end, we discussed what may be the issues and a plan.

 I was blindsided by the delays and did my own research. My best guess concluded we were most likely dealing with cerebral palsy. I learned from my research we could help her. I just needed someone to tell me how.
I was blindsided by the delays and did my own research. My best guess concluded we were most likely dealing with cerebral palsy. I learned from my research we could help her. I just needed someone to tell me how.

 Inspired by the success, I scoured the internet for a local baby music class. My web search led to a local non profit organization called
Inspired by the success, I scoured the internet for a local baby music class. My web search led to a local non profit organization called 

 learned to open her mouth to vocalize sounds, she grunted to fill in a pause while the therapist sang. Now, she tries to fill in a missing word with the few sounds she has mastered. Charlie started “singing” before she tried to talk.
learned to open her mouth to vocalize sounds, she grunted to fill in a pause while the therapist sang. Now, she tries to fill in a missing word with the few sounds she has mastered. Charlie started “singing” before she tried to talk.



 A year has passed since we have stayed in a hotel with Charlie. She is scared of the elevator and is obsessed with the trashcan. Overall, she’s been well behaved. I can contribute much of that to the indoor pool and Charlie’s swim class.
A year has passed since we have stayed in a hotel with Charlie. She is scared of the elevator and is obsessed with the trashcan. Overall, she’s been well behaved. I can contribute much of that to the indoor pool and Charlie’s swim class. activities and songs from swim class. Charlie gleamed as they played. She showed how she could splash, kick, and “swim”. I showed her dad how to hold her in the pool. I know it sounds ridiculous. But, without the class, I don’t think we would have known how to get anything out of pool time with Charlie.
activities and songs from swim class. Charlie gleamed as they played. She showed how she could splash, kick, and “swim”. I showed her dad how to hold her in the pool. I know it sounds ridiculous. But, without the class, I don’t think we would have known how to get anything out of pool time with Charlie.

 3) Cups
3) Cups  5) Squeaky Animals and Ninja Ducks Charlie loves her small rubber squeaky toys and ninja ducks. She will be receiving more of these.
5) Squeaky Animals and Ninja Ducks Charlie loves her small rubber squeaky toys and ninja ducks. She will be receiving more of these. 8) Shakers Charlie loves the maracas at music therapy. This idea was drawn from that.
8) Shakers Charlie loves the maracas at music therapy. This idea was drawn from that.











